Muriuki, JM;
Mentzer, AJ;
Webb, EL;
Morovat, A;
Kimita, W;
Ndungu, FM;
Macharia, AW;
Crane, RJ;
Berkley, JA;
Lule, SA;
et al.
Muriuki, JM; Mentzer, AJ; Webb, EL; Morovat, A; Kimita, W; Ndungu, FM; Macharia, AW; Crane, RJ; Berkley, JA; Lule, SA; Cutland, C; Sirima, SB; Diarra, A; Tiono, AB; Bejon, P; Madhi, SA; Hill, AVS; Prentice, AM; Suchdev, PS; Elliott, AM; Williams, TN; Atkinson, SH
(2020)
Estimating the burden of iron deficiency among African children.
BMC Medicine, 18 (1).
p. 31.
ISSN 1741-7015
https://doi.org/10.1186/s12916-020-1502-7
SGUL Authors: Crane, Rose Julia
|
PDF
Published Version
Available under License Creative Commons Attribution. Download (2MB) |
||
|
Microsoft Word (.docx) (Additional file 1)
Supporting information
Download (17kB) |
||
|
Microsoft Word (.docx) (Additional file 2)
Supporting information
Download (17kB) |
||
|
Microsoft Word (.docx) (Additional file 3)
Supporting information
Download (24kB) |
||
![[img]](https://openaccess.sgul.ac.uk/118503/6.hassmallThumbnailVersion/12916_2020_1502_MOESM4_ESM.png)
|
Image (PNG) (Additional file 4)
Supporting information
Download (405kB) | Preview |
|
![[img]](https://openaccess.sgul.ac.uk/118503/7.hassmallThumbnailVersion/12916_2020_1502_MOESM5_ESM.png)
|
Image (PNG) (Additional file 5)
Supporting information
Download (78kB) | Preview |
|
![[img]](https://openaccess.sgul.ac.uk/118503/8.hassmallThumbnailVersion/12916_2020_1502_MOESM6_ESM.png)
|
Image (PNG) (Additional file 6)
Supporting information
Download (165kB) | Preview |
|
![[img]](https://openaccess.sgul.ac.uk/118503/9.hassmallThumbnailVersion/12916_2020_1502_MOESM7_ESM.png)
|
Image (PNG) (Additional file 7)
Supporting information
Download (68kB) | Preview |
Abstract
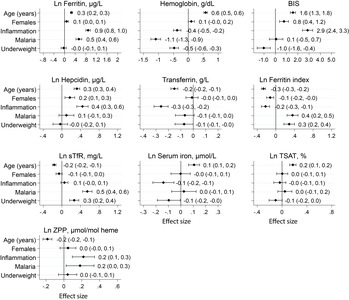
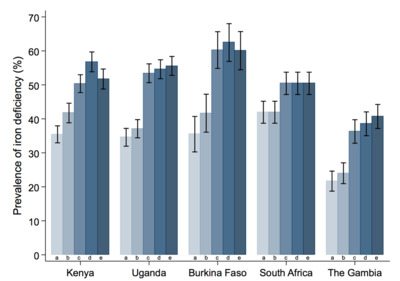
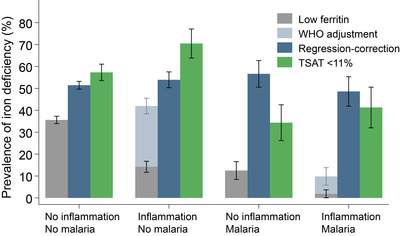
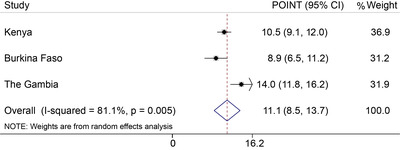
Background Iron deficiency (ID) is a major public health burden in African children and accurate prevalence estimates are important for effective nutritional interventions. However, ID may be incorrectly estimated in Africa because most measures of iron status are altered by inflammation and infections such as malaria. Through the current study, we have assessed different approaches to the prediction of iron status and estimated the burden of ID in African children. Methods We assayed iron and inflammatory biomarkers in 4853 children aged 0–8 years from Kenya, Uganda, Burkina Faso, South Africa, and The Gambia. We described iron status and its relationship with age, sex, inflammation, and malaria parasitemia. We defined ID using the WHO guideline (ferritin < 12 μg/L or < 30 μg/L in the presence of inflammation in children < 5 years old or < 15 μg/L in children ≥ 5 years old). We compared this with a recently proposed gold standard, which uses regression-correction for ferritin levels based on the relationship between ferritin levels, inflammatory markers, and malaria. We further investigated the utility of other iron biomarkers in predicting ID using the inflammation and malaria regression-corrected estimate as a gold standard. Results The prevalence of ID was highest at 1 year of age and in male infants. Inflammation and malaria parasitemia were associated with all iron biomarkers, although transferrin saturation was least affected. Overall prevalence of WHO-defined ID was 34% compared to 52% using the inflammation and malaria regression-corrected estimate. This unidentified burden of ID increased with age and was highest in countries with high prevalence of inflammation and malaria, where up to a quarter of iron-deficient children were misclassified as iron replete. Transferrin saturation < 11% most closely predicted the prevalence of ID according to the regression-correction gold standard. Conclusions The prevalence of ID is underestimated in African children when defined using the WHO guidelines, especially in malaria-endemic populations, and the use of transferrin saturation may provide a more accurate approach. Further research is needed to identify the most accurate measures for determining the prevalence of ID in sub-Saharan Africa.
| Item Type: | Article | ||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Additional Information: | © The Author(s). 2020 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated. | ||||||||||||||||||||||||||||||||||||
| SGUL Research Institute / Research Centre: | Academic Structure > Infection and Immunity Research Institute (INII) | ||||||||||||||||||||||||||||||||||||
| Journal or Publication Title: | BMC Medicine | ||||||||||||||||||||||||||||||||||||
| ISSN: | 1741-7015 | ||||||||||||||||||||||||||||||||||||
| Language: | en | ||||||||||||||||||||||||||||||||||||
| Publisher License: | Creative Commons: Attribution 4.0 | ||||||||||||||||||||||||||||||||||||
| Projects: |
|
||||||||||||||||||||||||||||||||||||
| Dates: |
|
||||||||||||||||||||||||||||||||||||
| URI: | https://openaccess.sgul.ac.uk/id/eprint/118503 | ||||||||||||||||||||||||||||||||||||
| Publisher's version: | https://doi.org/10.1186/s12916-020-1502-7 |
Statistics
Actions (login required)
 |
Edit Item |