Ellis, J;
Milburn, J;
Ngoni, K;
Williams, CG;
Muthoga, C;
Mwarumba, T;
Gwakuba, E;
Manenji, G;
Suresh, R;
Machiya, T;
et al.
Ellis, J; Milburn, J; Ngoni, K; Williams, CG; Muthoga, C; Mwarumba, T; Gwakuba, E; Manenji, G; Suresh, R; Machiya, T; Thubuka, J; Northcott, C; Penney, J; Kinsella, M; Mechie, I; Ensor, S; Leeme, T; Owen, L; Barton, H; Siamisang, K; Tenforde, MW; Hurt, W; Doyle, R; Grint, D; Molloy, SF; Harrison, TS; Goldfarb, DM; Mine, M; Mokomane, M; Ngwende, G; Gwaunza, L; Mazhani, T; Ndhlovu, C; Jarvis, JN
(2025)
Epstein-Barr Virus Central Nervous System Infections and Mortality Risk in Patients Presenting With Suspected Meningitis: Results From the Botswana National Meningitis Survey and the Harare Meningitis Aetiology Study.
Open Forum Infectious Diseases, 12 (12).
ofaf660.
ISSN 2328-8957
https://doi.org/10.1093/ofid/ofaf660
SGUL Authors: Molloy, Sile
Abstract
Background
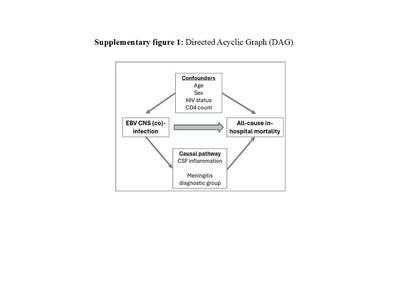
Epstein-Barr virus (EBV) central nervous system (CNS) infection in immunocompromised hosts and among meningitis cohorts is well recognized. The clinical significance of EBV CNS infection, however, is poorly understood.
Methods
Data were collected as part of the Botswana National Meningitis Survey and the Harare Meningitis Aetiology Study. The prevalence of EBV CNS infection (EBV DNA detected in cerebrospinal fluid [CSF] by means of quantitative polymerase chain reaction) was determined, alongside associations with baseline covariates and the in-hospital mortality rate.
Results
A total of 581 participants with suspected meningitis were recruited. Of these, 54% were male, the median age (interquartile range) was 38 (29–46) years, and 76% were persons living with human immunodeficiency virus (HIV). Cryptococcal meningitis was the most common microbiologically confirmed infectious meningitis (12.0%), and 6.4% of participants had definite tuberculous meningitis. EBV CNS infection was common (26% [152 of 581]) and was associated with older age, being HIV positive, and CSF pleocytosis (P < .001). It was also associated with increased in-hospital mortality rate (odds ratio, 1.64, [95% confidence interval, 1.10–2.43]; P = .01), but after adjustment for sex, age, and HIV status, there was no longer evidence of an association (adjusted odds ratio, 1.29 [.84–1.98]; P = .25). In subgroup analyses, there was an indication that the association between EBV CNS infection and mortality rate may differ by meningitis subgroup.
Conclusions
EBV CNS infection was common among our cohort, and it was strongly associated with CSF pleocytosis. Following multivariable analyses, EBV CNS infection overall was not associated with in-hospital mortality rate. EBV CNS infection in the context of meningitis is most likely a “bystander” virus that reflects heightened CSF inflammation.
Statistics
Item downloaded times since 11 Dec 2025.
Actions (login required)
 |
Edit Item |
![[img]](https://openaccess.sgul.ac.uk/118115/3.hassmallThumbnailVersion/ofaf660_supplementary_data.jpeg)